Recent advances of pharmacogenomics in severe cutaneous adverse reactions: immune and nonimmune mechanisms
Last Updated on September 26, 2016 by Joseph Gut – thasso

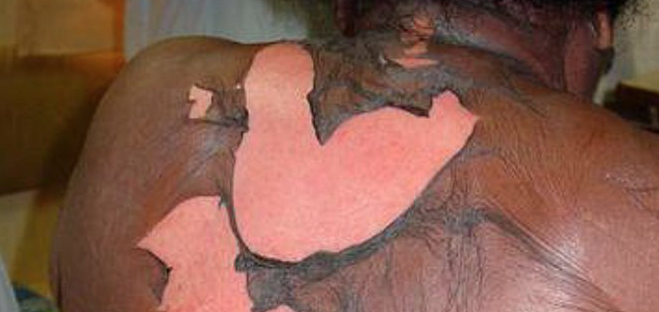
September 26, 2016 – Toxic epidermal necrolysis (TEN), also known as Lyell’s syndrome, is a rare, life-threatening skin condition that is usually caused by a reaction to drugs. The disease causes the top layer of skin (the epidermis) to detach from the lower layers of the skin (the dermis), all over the body, leaving the body susceptible to severe infection. The case fatality ratio ranges from 25 to 30%, and death usually occurs as a result of sepsis and subsequent multiorgan system failure. Treatment primarily involves discontinuing the use of causative agent(s), and supportive care in either the intensive care unit or burn unit of a hospital.
The publication below, by Dao et. al., gives an overview on the pharmagogenetic options that exist today to prevent Lyell’s syndrome, along with a selection of other very serious, if not fatal skin reactions, when genetically susceptible individuals are exposed to certain drugs.
Dao RL, Su SC, Chung WH
Asia Pac Allergy 2015 Apr;5(2):59-67
PMID: 25938070
Abstract
Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS) are severe cutaneous adverse reactions (SCAR) which are majorly caused by drugs. Though the incidence rate is low, SCAR sometimes can be life-threatening and leads to lifelong sequelae. Many pharmacogenomic associations in immune and nonimmune related genes with the development of SCAR have been discovered recently and the pharmacogenetic tests have been applied to prevent specific drug-induced SCAR. In this review, we discuss the recent advances of pharmacogenomics in SCAR.






